Artemisinin, long considered to be the miracle drug in the fight against malaria, is losing its grip on the disease in the Mekong region, but perhaps not for the reasons you might think. The science is still sound, and researchers and local groups still work around the clock to tackle the mosquito-borne disease. But the disease is developing resistance in the dense jungle environment of the Thai-Burmese border, an area that is poorly funded, and, on the Burmese side, the backdrop to decades of civil conflict that has pushed the treatment of the disease towards the bottom of the national priority list.
Fatalities from malaria have dropped substantially over the last 15 years, with the latest UN study reporting a 47 percent decline from 2000–14. This dramatic improvement has been largely attributed to Artemisinin-based combination therapies (ACTs), whereby partner drugs are delivered with Artemisinin, a Chinese herb derivative, which effectively combats the single cell parasite responsible for malaria: plasmodium. There are two major strains of the parasite: Vivax, the most common and somewhat easier to treat; and Falciparum, which can lead to brain damage if left unattended. Both strains have begun to demonstrate resistance to ACTs. The resistance was first detected in Cambodia, but has now made its way across our man-made borders into Burma. It’s this migration that has experts worried. If resistance spreads from Burma into neighbouring India and China, the consequences will be devastating.
Researchers at the Shoklo Malaria Research Unit (SMRU) have been working towards what they say is the only possible goal: complete elimination of malaria. Leader researchers Dr Francois Nosten and Gilles Delmas say that despite the success derived thus far from Artemisinin treatments, stalling and disorganisation on behalf of the international community has stymied opportunities to win the war permanently against the disease.
“We are busy with a program of elimination – which is trying to move faster than the resistance … and eliminate the parasite before it becomes completely resistant to the Artemisinin and to the [accompanying] partner drugs,” Dr Nosten said from the SMRU office in Mae Sot.
When asked about the support from the WHO, Dr Nosten did not offer a ringing endorsement.
“It has been very disappointing over the years … this [Artemisinin resistance] is not a new problem. It emerged in 2007 – it is now 2015. A lot of meetings, but not much is [being done] in the field in the [Mekong] region. Why? To put it bluntly, it is because WHO are not doing their job … they didn’t play the role that people expect them to play. Being the world organisation that looks after the health problems of the world … they have made a lot of plans and published objectives and reports, but not a lot in terms of action.”
But Nosten’s perception of the WHO response seems to run contrary to the WHO’s self-review. The health arm of the United Nations publishes a malaria report annually in December, with the 2014 edition citing an overall dramatic decrease in the disease burden and a global reduction of the disease incidence of some 30 percent, and a significant 54 percent decline in Africa.
Representatives at WHO were contacted directly to respond to these issues, but at the time of print had not made a statement.
But these promising figures bely the brewing danger in the Mekong region, and the concern held by those on the ground is that should the resistance spread to India, it will be too late to prevent a migration to Africa. It is this scenario that SMRU and other experts in the region are desperate to avoid. Mr Delmas is working with local community health groups to set up and expand a series of ‘malaria posts’ – small health centres that focus entirely on detecting malaria, and then treating it. Manned almost entirely by villagers, the programme helps keep malaria incidence rates from rising, as well as giving locals training and assistance to maintain autonomy over the health of their own communities.
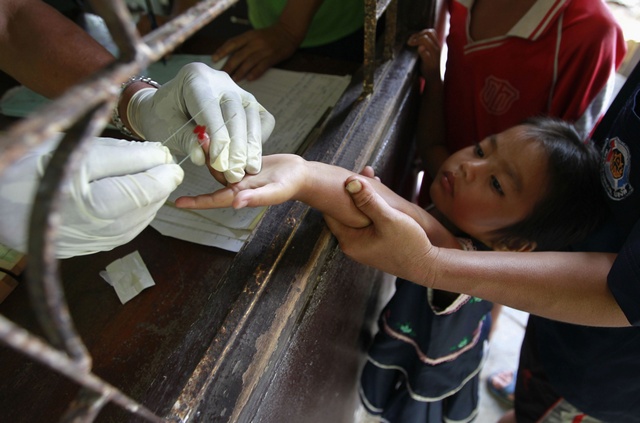
Within the first 24 hours of suspected symptoms, villagers can present to the outposts and receive a simple pinprick rapid diagnostic test (RDT). Results are evident on the RDT within 15 minutes. With treatment beginning immediately, the patient will no longer pose a risk as a ‘malaria reservoir’, as Delmas puts it. More than 500 posts are in currently in operation along the border, with more planned over the coming year.
The Karen Health and Welfare Department (KDHW) run such malaria posts in local Karen areas, in addition to their own programmes of malaria treatment and education. Karen State territory begins directly on the porous Thai-Burmese border, and the Karen people see first-hand the devastating and prolonged effects that persistent malaria has had on their people. Despite significant funding limitations, Saw Diamond from the KDHW says that combating malaria is their responsibility, and one that they take very seriously.
“Within six months of starting our first malaria survey in 2003, we saw prevalence decrease in our communities. One in ten villagers has the parasite but shows no symptoms … We have to work hard to ensure testing and education is one of the key focuses, so the parasites cannot spread to those with a poor immune system,” Saw Diamond said.

Infants, the elderly and the sick often develop symptoms along with infection, but adults with a strong immune system can carry the parasite for months, even years, without showing any signs. In this way, many are unwittingly the ‘reservoirs’ Mr Delmas refers to.
The constant clash between ethnic groups and government forces, and the resultant thousands of villagers that are consequently displaced, makes it even more difficult to maintain control over a disease that transcends arbitrary borders and territories. “If we don’t do it, nobody else can,” says KDHW’s Saw Diamond.
Prior to 2012 there was no collaboration between the central Burmese government and KDHW, or other grassroots groups working on malaria treatment and elimination. Further, some villages refuse collaboration while hostilities still flare. The northern township of Hpapun [Papun] in Karen State steadfastly refuses any resources that come from Naypyidaw.
The KDHW are more receptive to teamwork with the government, but make clear that the goal is elimination, and nothing further: “[We] are very happy to work [with the government] towards no malaria in all of Burma. But, we don’t want to make propaganda for their political gains.”
The real extent of governmental support is hard to confirm. Ethnic groups are protective of their work within their communities, and at the time of print, requests for comment to the Ministry of Health had not been returned.
In the US last month, the University of Maryland hosted the ‘Working together to eliminate Malaria in Myanmar’ conference – a joint partnership with a variety of international partners, including the Bill and Melinda Gates Foundation. It was attended by several of Burma’s ethnic groups, government health representatives, military representatives, and NGOs. Both SMRU and the KDHW agree the conference made some gains, but fear the summit was more an exercise in publicity rather than a tacit programme of tangible goals.
Sources say that the military presence at the August meeting were largely amenable to suggestions, but balked at terms that identified ethnic groups specifically, saying that “national race” is the preferred reference.
As with all development projects, access to adequate and reliable funding is often a game-changing factor in the efficacy of any large-scale undertaking. The Global Fund, an international financing organisation specifically focused on combatting malaria, tuberculosis and AIDS, is working in tandem with partners in the border region, backing the village health centres and providing much needed infrastructure.
Izaskun Gaviria, a senior fund manager in the Global Fund Asia division, identified some of the same challenges as Dr Nosten and the KDHW – particularly, the inability of the Burmese government to effectively absorb and distribute funding.
“The challenges are of course insecurity, bad infrastructure, poor communication and lack of internet connectivity. The constant staffing changes occurring at the Ministry of Health have an impact on the programmes too, hence implementation and expansion, and thus budget absorption, do not happen rapidly,” Gaviria said.
Despite these practical setbacks, money funneled directly to the villages was not only having an effect, Gaviria said, it is exceeding expectations.
“Over 10,000 VHV [village health volunteers], supported solely by Global Fund finance, are active now and their performance is very good – they have exceeded the target set for them in 2015 and so we will expand more.”
[related]
The stories on the ground seem to echo one another: give the people squaring off with the threat of a burgeoning malaria resistance what they need; give them autonomy over their own health projects, and amazing things happen. Saw Diamond and his team, and other ethnic groups in Burma are clearly taking this threat seriously, and they are making equally serious strides in bringing it back under control.
The progress always seems to stall at a bureaucratic level.
Malaria doesn’t abide by arbitrary timelines and borders. It doesn’t care about ethnic conflicts, about changes in the ministry, or about whether the villages are adequately prepared. It certainly doesn’t care about who is in power from the relative comfort of Naypyidaw, or who is making the calls in Geneva.
A follow up to the Maryland conference is due later in the year, and the Ministry of Health is set to join some of the ethnic groups in the SMRU office next month to share data. But with the Burmese election looming, meetings are far from set in stone. When asked how the election result could impact the battle against malaria, Dr Nosten was tentative.
“It doesn’t matter who is in control … what matters is that we can eliminate malaria. That is the objective.