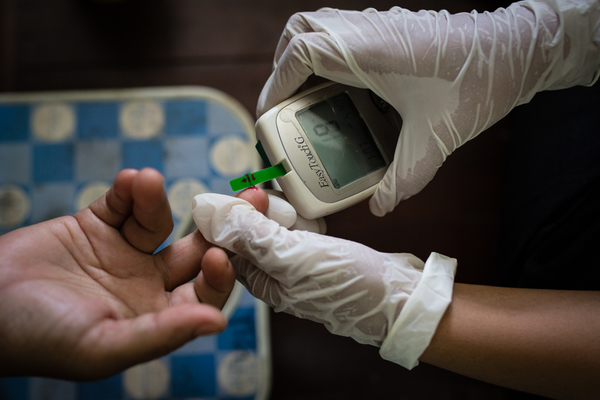
At a mobile clinic in East Dagon, a 27-year-old female patient with early diabetes is about 16 weeks pregnant. Few weeks ago, a doctor prescribed her oral hypoglycemic agents that would be safe to take during the pregnancy. However when she went to a pharmacy for refills, she received a different, contraindicated drug.
May Kyaw Thet, a doctor at the clinic run by the local NGO Better Burmese Health Care, would like to switch the patient to insulin injections, but she doesn’t have a refrigerator at home. The clinic could supply an icebox, but that will need to be replenished every couple of days at a cost of about 200 kyats, which the patient cannot afford. The management of diabetes, relatively simple in developed countries, is complicated by lack of access to medical services, low health literacy and poverty in Burma.
Situations like these provide a glimpse into a large and growing health threat within Burma. As of 2013, the International Diabetes Federation Atlas puts diabetes prevalence in Myanmar among people aged between 20 and 79 at at 5.8 percent.
Based on a Rangoon-only sample, a WHO study in 2003-2004 found 11.8 percent prevalence. While the later number “doesn’t represent the whole country”, said Dr Ko Ko, part of a diabetes prevention project of the Myanmar Society of Endocrinologists and Metabolism, the numbers are concerning as more people settle in cities, adopt sedentary lifestyles and consume more fast foods on top of an average diet that consists of up to 75 percent white rice, a food that’s high on the glycemic index. “We need to know the magnitude of the problem,” he said “how much it has economic impacts. To get accurate data is very much important for us to show the public, government and parliament.”
[related]
Do Ko Ko is undertaking a new survey of 9300 people in 52 townships that will be completed by March 2015. He said he expects the current countrywide diabetes prevalence to be around 6 percent and hypertension (high blood pressure) to be around 30 percent. The latter can lead to or complicate forms of diabetes.
On 14 November, International World Diabetes Day, he will give a public lecture to over 500 people in Naypyidaw, on the symptoms of diabetes and its treatment and risk factors. The lecture will be followed by an event of free blood-sugar and body-fat screenings.
Dr Ko Ko said that “by modifying environmental factors such as cutting out on an unhealthy diet and lack of physical activities,we can prevent DM by 58% [according to]evidence-based data.”
For its part, Better Burmese Health Care doctors see over 11,400 patients each year through their mobile clinics in East and South Dagon. About 85 percent are diabetic and over 90 percent patients have hypertension.
When Dr Jalin Sama founded the NGO in 2008 to provide humanitarian reliefcare in the wake of Cyclone Nargis, the doctors had not predicted that diabetes would become the center of their focus.
“We were simply responding to the needs of the Nargis victims,” Dr Sama said.“We just happened to notice high rates of diabetes mellitus and started focusing on managing and treating it.”
Poverty and lack of health education in Burmahas made this work a challenge. “Many people with Type 2 diabetes do not have the appropriate knowledge to manage the disease,” Dr Sama said. As such, doctors at the clinic have incorporated group education about diet, physical activity, mindfulness and well being, as also compliance with drug treatment into the clinic program.
However, since diabetes does not cause immediate health problems the way tuberculosis or malaria does, doctors find it hard to persuade patients to accept treatment or even to modify their lifestyle.
“That’s partly understandable,” said Dr Sama ,since following a healthy lifestyle can be “a tremendous financial burden” on patients. “Vegetables and meat are expensive. Medications are expensive. Access to health facilities is difficult.”
Without a health insurance system, patients must pay out of pocket for everything.“There’s no funding for non-communicable diseases,” Dr Ko Ko said. “Many donor countries donate only towards communicable diseases. And we cannot control [the availability of] soft drinks,alcohol, tobacco and palm oil, although we are trying.”
Although diabetes is non-communicable, depending mostly on genetic and lifestyle factors, it causes immunodeficiency in patients increasing their vulnerability to contracting communicable diseases. A recent study in The Lancet has placed Myanmar among the top 10 countries in the world with the highest rates of diabetes-related tuberculosis, with 21,000 cases. The study has pointed out that in order to achieve complete success in eliminating TB on a worldwide scale, it is important to tackle diabetes.
“Ameliorating high rates requires a multi-prong approach,” Dr Sama said. She suggestedpublic awareness campaigns at the national level, proper or upgraded training of health-care personnel and making it easy to access care.
Supported by the Ministry of Health, efforts to tackle diabetes have begun. Dr Ko Ko said the diabetes prevention project is training around 50 health-care workers each year and monthly public education sessions will be a focus of 2015.